Medication cost is the leading reason prescriptions go unfilled in the U.S.*
Source: GoodRx
Simply put, when cost becomes a barrier, care stops. It is a key predictor of whether a patient will start treatment and whether they will stay on it. Sudden insurance changes, high out-of-pocket costs, and unclear or shifting coverage rules can make the difference between a therapy being within reach or effectively impossible to start or maintain. Even small increases in cost burden can reduce adherence, widen inequities, and push manageable chronic conditions into crisis. When affordability breaks down, clinically appropriate prescriptions turn into abandoned treatment plans.
For too many Americans, affordability concerns often force them to make impossible tradeoffs between basic necessities like food and shelter and essential medicines for themselves or their families. This is exacerbated by a complex healthcare system that often lacks transparency around how medicines are priced and what patients are ultimately expected to pay.
Americans leave their prescription at the pharmacy every month, mainly due to cost:
46,000,000Source: GoodRx
More than half of adults in America say they have not filled or taken full prescription dosage because of the cost
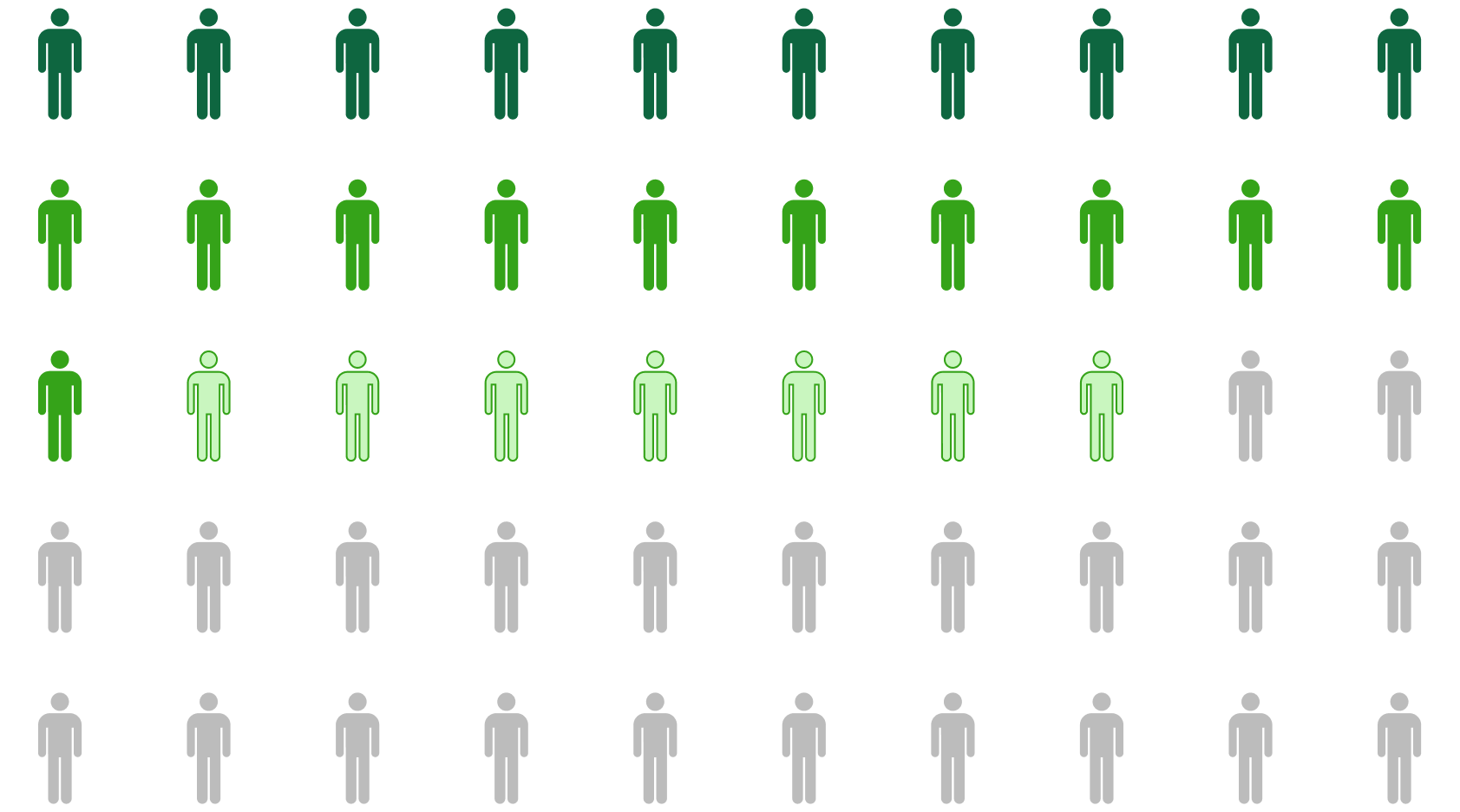
Source: Kaisr Family Fundation
Proportion of Americans who filled a prescription in 2025 who said it created at least a minor financial burden
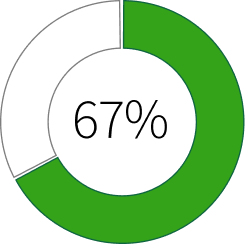
Source: Kaisr Family Fundation
Proportion of adults who say they skipped or postponed getting health care they needed because of the cost in the past year
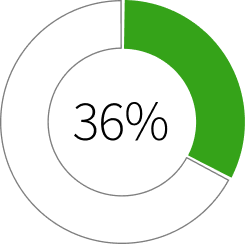
Source: GoodRx
There has been much debate and scrutiny around prices that drug manufacturers set, and that is an important consideration. But there are also several other forces that can have a huge impact on determining a patient’s actual cost, including intermediary costs, insurance coverage, and regulations. Together, these elements reveal where barriers emerge, where support is needed, and where targeted interventions can reduce financial strain and help keep treatments within reach.
